PRP Treatment Near Troy MI
In Troy, MI, you can get platelet-rich plasma (PRP) at Michigan Center For Regenerative Medicine as an outpatient procedure using a small draw of your own blood that’s centrifuged to concentrate platelets and growth factors, then injected into a joint, tendon, or scalp under sterile technique, often with ultrasound guidance.
Learn more about Platelet Rich Plasma Therapy.
You’ll likely feel soreness for 24–72 hours, avoid NSAIDs if advised, and start noticing improvement in 2–6 weeks, with peak benefit around 8–12+ weeks. Next, you’ll see who’s a good candidate, the costs, and session planning.
Main Takeaways
- PRP may be deferred for active infection, significant bleeding risk, uncontrolled illness, severe end-stage arthritis, or platelet/blood disorders.
- PRP treatment in Troy, MI is an outpatient procedure using your own concentrated platelets to support tissue repair and pain reduction.
- Common uses include knee osteoarthritis, tendon/ligament injuries, and select dermatology needs like hair thinning and acne-scar remodeling.
- Visits typically include screening, medication review, and often ultrasound-guided injection for accurate, sterile placement.
- Expect soreness for 1–3 days; improvements often begin 2–6 weeks after treatment and peak around 8–12+ weeks.
To learn more about PRP treatment near Troy MI, call The Michigan Center for Regenerative Medicine today at (248) 216-1008.
Ask About Alternatives to Surgery for Your Chronic Pain
Contact the Michigan Center for Regenerative Medicine Today and Schedule Your Office Visit
PRP Treatment in Troy, MI: What It Is
Platelet-rich plasma (PRP) therapy uses a concentrated portion of your own blood, rich in platelets and growth factors, to support tissue repair. In Troy, MI, you’ll typically receive PRP as an outpatient procedure used in orthopedics, sports medicine, and some dermatologic protocols when conservative care hasn’t met goals.
PRP uses your own platelet-rich blood to support tissue repair, often offered outpatient in Troy for ortho, sports, and select dermatology needs.
You’ll start with a brief medical screening to confirm indications, review medications, and set realistic expectations.
A clinician draws a small blood sample, then spins it in a centrifuge to separate and concentrate platelet-rich plasma.
The team then prepares the target site using standard sterile technique and may use ultrasound guidance to improve placement accuracy. Because protocols vary, you’ll ask how PRP is prepared, what dose is used, and how outcomes are tracked. This helps you avoid treatment misconceptions driven by marketing claims.
With clear counseling, you can serve others by choosing care grounded in evidence and safety.
What PRP Actually Does After Injection
After your clinician places PRP into the target tissue, the concentrated platelets activate and release signaling proteins (growth factors and cytokines) that modulate local inflammation and recruit repair cells.
You’re not getting a “filler”; you’re delivering a biologic cue that shifts the microenvironment toward regulated repair. Next, platelet proteins support Inflammation modulation by tempering excessive inflammatory signaling while still permitting the early cleanup phase.
You can expect a short-lived soreness as immune cells clear damaged matrix and prepare a scaffold for repair. As signaling continues, you promote fibroblast activity and collagen organization, helping tissue remodel along functional lines. PRP also drives Angiogenesis promotion, improving microvascular supply so oxygen and nutrients reach the repair zone more efficiently.
Over days to weeks, you’ll see a progression from inflammatory to proliferative and remodeling phases, guided by your body’s own pathways. You support this process by following post-procedure load, rest, and rehab instructions closely.

What PRP Can Treat (Joints, Tendons, Hair)
You can use PRP to target joint pain and osteoarthritis by injecting platelet-rich plasma into the affected joint under sterile technique, often with imaging guidance. You can also treat select tendon and ligament injuries with precisely placed injections to support tissue repair and reduce pain.
You can address hair thinning and loss by delivering PRP into the scalp in a structured series to stimulate follicles and improve hair density.
Joint Pain And Arthritis
When joint cartilage and surrounding soft tissue start breaking down, chronic inflammation and mechanical stress can drive persistent pain and stiffness.
If you’re serving others, you can’t afford unreliable knees, hips, or shoulders, so you’ll want a structured plan that targets function, not just symptoms. PRP may help mild-to-moderate osteoarthritis by delivering concentrated platelets and growth factors to support a healthier joint environment and pain reduction.
Your clinician will confirm diagnosis with history, exam, and imaging, then draw blood, process it, and use ultrasound-guided injection into the joint.
You’ll follow post-procedure loading guidance with Exercise modifications and progressive strengthening, plus Nutrition strategies that support weight management and metabolic health.
You’ll track outcomes with pain scores, range of motion, and activity tolerance over 6–12 weeks.
Tendon And Ligament Injuries
Joint-focused PRP can reduce pain and improve function in mild-to-moderate osteoarthritis, but many persistent pain problems come from tendons and ligaments rather than the joint surface itself.
If you’re supporting others through chronic overuse or acute strain, you’ll want a plan that targets the injured tissue and restores load tolerance.
You’ll start with a biomechanical assessment to identify faulty mechanics, training errors, and contributing weakness. Then you’ll undergo image-guided PRP injection into the involved tendon or ligament to concentrate growth factors at the repair site.
Evidence suggests PRP can help conditions like lateral epicondylitis, patellar tendinopathy, Achilles tendinopathy, and partial ligament sprains when rehab alone stalls. You’ll pair treatment with progressive loading, activity modification, and preventive exercises to reduce recurrence and protect your service capacity.
Hair Thinning And Loss
Although PRP is widely used for musculoskeletal repair, it can also address hair thinning by delivering concentrated, autologous growth factors to the scalp to support follicle function. You’ll start with a focused evaluation of shedding pattern, lab contributors, and Genetic predisposition, then your clinician prepares PRP from your blood and injects it intradermally across thinning zones.
| What you assess | What PRP targets |
|---|---|
| Miniaturization pattern | Follicle cycling support |
| Inflammation signals | Scalp microbiome balance |
| Treatment response | Density and caliber |
You’ll typically complete a series of sessions spaced weeks apart, then maintain periodically. You can serve others best when you stay consistent: avoid traction, optimize nutrition, and document photos under the same lighting. Expect gradual change over months, with outcomes varying by stage and adherence.

PRP for Joint Pain in Troy: Who Benefits Most
If you’re considering PRP for joint pain in Troy, you’ll benefit most when you have mild-to-moderate degenerative changes, localized symptoms, and you can follow a structured rehab plan.
Your clinician will screen you for ideal candidacy by confirming a clear pain generator, reviewing imaging and prior conservative treatments, and ruling out contraindications such as active infection, significant bleeding risk, or severe end-stage arthritis.
PRP tends to help most in knee osteoarthritis and select hip, shoulder, and ankle joint pain cases where inflammation and cartilage wear drive symptoms rather than unstable mechanical damage.
Ideal Candidates For PRP
Because PRP uses concentrated platelets to support tissue repair and modulate inflammation, the best candidates tend to share specific clinical features. You’re a strong candidate when you have localized pain, stable function, and realistic expectations for gradual improvement.
You’ll complete a focused exam, imaging as indicated, and a medication review to reduce medication interactions (especially anticoagulants and NSAIDs). You may not qualify if you have active infection, uncontrolled systemic illness, or blood disorders that impair platelet function.
| Screening step | What you report | Clinician action |
|---|---|---|
| History | pain pattern, prior care | define target, rule red flags |
| Meds | NSAIDs, anticoagulants | plan hold/bridge if appropriate |
| Labs | anemia, platelet issues | confirm safety; defer if needed |
| Goals | service-ready function | set timeline, rehab plan, follow-up |
Conditions PRP Helps Most
Once you’ve confirmed you’re a good candidate, the next step is matching PRP to the condition most likely to respond.
You’ll see the strongest evidence in mild to moderate knee osteoarthritis, where PRP can reduce pain and improve function for months.
You may also benefit with tendinopathies (lateral epicondylitis, patellar, Achilles) and ligament sprains when you’ve failed structured rehab and need biologic support.
Your clinician should use ultrasound guidance, document baseline scores, and pair injections with progressive loading.
For skin and wound care, you can consider PRP for Acne scarring when you combine it with microneedling or laser to support collagen remodeling.
You may use PRP adjunctively for Diabetic ulcers under multidisciplinary offloading, infection control, and glycemic optimization.
PRP for Tendon Injuries in Troy: Common Conditions
When does PRP make the most sense for tendon pain in Troy?
You’ll consider it when symptoms persist beyond 6–12 weeks despite activity modification, targeted loading, and physical therapy.
Consider PRP when tendon pain lasts 6–12+ weeks despite activity modification, targeted loading, and consistent physical therapy.
Clinical Evidence supports PRP most consistently for chronic tendinopathies rather than acute tears, and you’ll weigh Occupational Impact when pain limits lifting, gripping, climbing, or patient-handling duties.
Common tendon conditions you may treat include lateral epicondylitis (tennis elbow), medial epicondylitis, patellar tendinopathy, Achilles tendinopathy (mid-portion), proximal hamstring tendinopathy, gluteal tendinopathy (greater trochanteric pain), and rotator cuff tendinopathy without full-thickness rupture.
Procedurally, you’ll confirm diagnosis with exam plus ultrasound or MRI, then use ultrasound-guided injection into the degenerative portion, avoiding intratendinous anesthetic.
You’ll follow a staged rehab plan with relative rest, then progressive eccentric/concentric loading and return-to-service criteria.

PRP Hair Restoration in Troy: What to Expect
PRP doesn’t only target chronic tendon degeneration, it’s also used to support hair follicle function in patients with thinning hair in Troy.
You can expect a candid review of your hair-loss pattern, medical history, medications, and scalp health to confirm you’re an appropriate candidate.
Evidence suggests PRP may improve hair density and shaft caliber in androgenetic alopecia when delivered in a structured series and paired with consistent home care. You’ll discuss realistic goals, time to response (often months), and the need for maintenance sessions.
You’ll also review risks such as temporary soreness, pinpoint bleeding, headache, or no meaningful change, plus contraindications like active scalp infection or certain bleeding disorders. You should plan ahead for appointment scheduling and parking logistics so you can arrive unhurried and keep your focus on serving others.
Expect baseline photos and objective measurements to track change over time accurately.
Your PRP Appointment in Troy: Step-by-Step
You’ll start with pre-visit preparation, where you review medications and supplements and follow clinic instructions to reduce bleeding risk and optimize platelet yield.
During the procedure, you’ll have a brief blood draw, PRP processing by centrifugation, and targeted injections performed under sterile technique with pain-control options as needed. Afterward, you’ll follow a structured aftercare plan and schedule follow-up visits to monitor response and determine whether additional sessions are indicated.
Pre-Visit Preparation
Before your Troy PRP appointment, follow a short, medication-aware checklist to optimize platelet function and reduce avoidable bruising or swelling.
Review all prescriptions, supplements, and OTC pain relievers with your clinician; don’t stop anticoagulants or antiplatelets unless your prescriber directs it. If allowed, avoid NSAIDs for several days pre-visit; acetaminophen is often preferred for discomfort.
Limit alcohol and nicotine, hydrate well, and eat a balanced meal unless you’re told to fast.
Bring a document checklist: ID, insurance card, medication list, allergies, prior imaging, and relevant medical records. Complete consent and intake forms early to respect staff time. Do transportation planning if a treated joint may feel sore afterward.
Wear loose, easy-access clothing.
During The Procedure in Troy
On arrival at your Troy visit, the team confirms your identity, reviews your medical history and medication list, and documents baseline pain and function for the target area.
You’ll enter a prepared room with ambient lighting and optional procedure music to support calm focus. The clinician positions you to protect the joint or tendon and cleans the skin using sterile technique. You’ll have a venipuncture to collect blood, then staff centrifuge it to concentrate platelets per protocol. If indicated, you’ll receive local anesthetic, selected to minimize platelet exposure.
Using ultrasound guidance, the clinician identifies the target, avoids neurovascular structures, and advances a needle with real-time visualization. You’ll feel pressure or brief discomfort as PRP is injected, then the site is dressed.
Aftercare And Follow-Up in Troy
Once the injection is complete, the clinician monitors you briefly, reviews expected post-procedure soreness and swelling, and confirms there’s no concerning bleeding, dizziness, or allergic response.
You’ll leave with clear activity limits and a plan to protect the treated area so you can keep serving others safely and consistently.
- Use ice and elevation as instructed, and avoid NSAIDs unless your clinician approves; they may blunt the intended inflammatory response.
- Start Symptom Tracking daily: pain level, stiffness, bruising, and function, plus any changes in sleep or energy.
- Watch for Emergency Signs: rapidly expanding swelling, fever, drainage, severe redness, chest pain, shortness of breath, or fainting, seek urgent care.
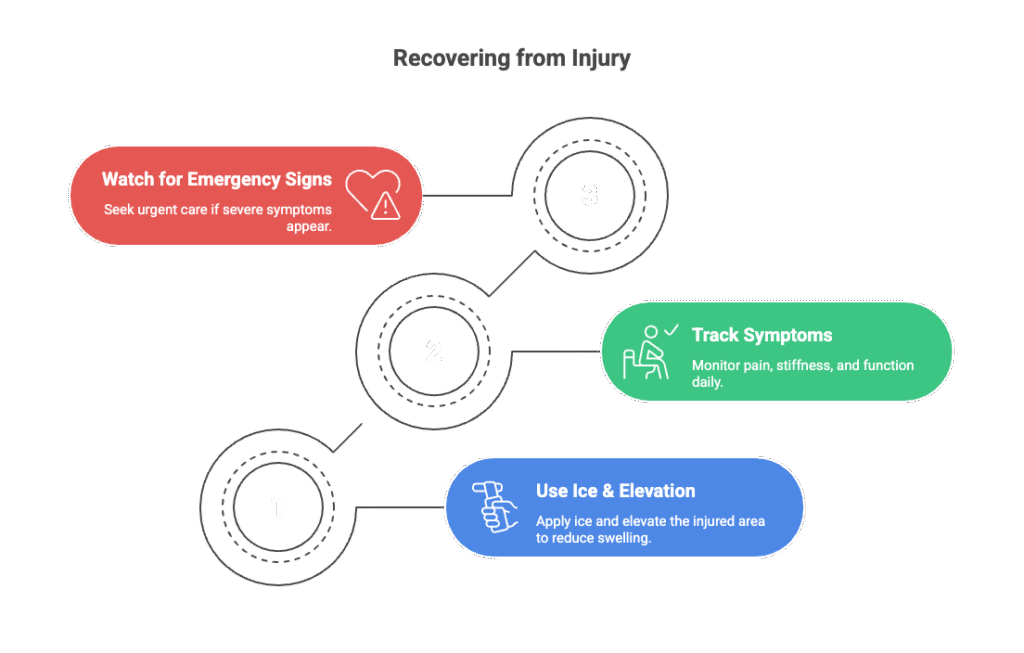
Schedule follow-up for reassessment, rehab progression, and deciding if additional PRP sessions are appropriate.
Downtime, Side Effects, and Safety of PRP
Although PRP uses your own platelets, you should still plan for brief downtime and understand the expected side effects and safety profile.
Even with your own platelets, PRP can mean brief downtime—know the typical side effects and safety basics first.
Most people return to light activity the same day, but you’ll often need to limit strenuous exercise for 24–48 hours and follow site-specific restrictions to protect recovering tissues. Expect transient soreness, swelling, warmth, bruising, and a “full” sensation; these typically peak within 24–72 hours and then resolve.
You can usually use acetaminophen for discomfort; avoid NSAIDs if your clinician advises, since they may blunt inflammation signaling. Safety depends on sterile technique, proper centrifugation, and clear Regulatory oversight for collection and handling.
Because PRP is autologous, Allergy risks are low, but you can still react to antiseptics, latex, or added anesthetics. Call promptly for fever, spreading redness, drainage, severe pain, or neurologic changes.
How Many PRP Sessions Do You Need in Troy?
- Initial session: You’ll complete imaging review, baseline pain/function scores, and ultrasound-guided placement to target the involved tissue precisely.
- Reassessment window: You’ll return for repeat exam and outcome measures; if strength, range, and task tolerance improve, you may pause and continue rehab.
- Additional sessions: If progress plateaus or the lesion is extensive, you may receive 1–2 more injections spaced per protocol. These will be paired with activity modification.
Clinics may offer Package options. But you should anchor decisions to documented response, safety screening, and your commitment to return-to-service duties and sustained rehab.
Cost, Results Timeline, and Choosing a Troy Provider
After you’ve set expectations for how many PRP sessions you may need, you should map out three practical variables: total cost, the results timeline, and the provider’s protocol quality in Troy. You’ll typically self-pay; ask about Insurance Coverage only for PRP-related imaging, consults, or bracing. Request an itemized quote (draw, processing kit, ultrasound guidance, post-care) so you can budget responsibly while staying focused on returning to service.
| Variable | What to Ask | Practical Target |
|---|---|---|
| Total cost | Itemized fees, bundles | Transparent, no add-ons |
| Timeline | When improvement starts | 2–6 weeks |
| Peak benefit | When outcomes stabilize | 8–12+ weeks |
| Monitoring | Recheck plan, outcomes | Scheduled follow-ups |
| Protocol quality | Processing, guidance, rehab | Standardized, documented |
To choose well, verify Provider Credentials (board certification, PRP experience, ultrasound training) and ask for protocol details: platelet concentration method, activation plan, sterile technique, and rehab integration. You’re protecting patients and your own readiness.

If you’re considering PRP treatment in Troy, MI, you’ll start with an exam, imaging review, and goal setting at Michigan Center For Regenerative Medicine. Your provider will draw blood, concentrate platelets, and inject PRP using sterile technique, often with ultrasound guidance.
You can expect mild soreness and a need to modify activity for several days.
Most protocols use 1–3 sessions, spaced weeks apart, with results developing over 4–12 weeks. To learn more, visit Platelet Rich Plasma Therapy. Choose a qualified clinician and discuss realistic outcomes, risks, and total cost.
Here at the Michigan Center for Regenerative Medicine, we talk with patients every day who have long-term pain, discomfort and physical disabilities due to injury. As While it’s true that platelets clot the blood, they also are comprised of several proteins known as growth factors that are critical in the healing of injuries, according to the American Academy of Orthopaedic Surgeons.
Contact the Michigan Center for Regenerative Medicine at (248) 216-1008 about PRP treatment near Troy MI.




A Solution for Chronic Pain Management
PRP, a trusted treatment in sports medicine for decades, has been helpful in getting athletes to heal more readily after injury. Speedier wound healing and bone-grafting processes in the fields of neurosurgery, maxillofacial surgery, otolaryngology and orthopedic surgery are additional benefits to PRP treatment near Troy MI.
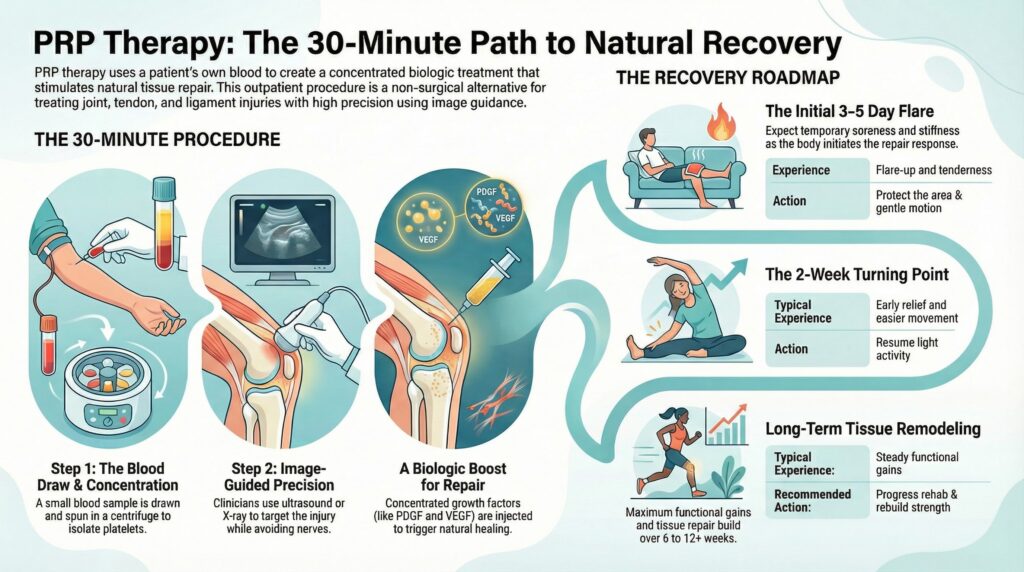
Upon offering your blood sample, it takes just 30 minutes to prepare your treatment. Featuring minimal risks and exceptional effectiveness rates, PRP follows a simple process:
- Platelets become separated aside from other blood cells and concentrated with centrifugation.
- The concentrated platelets are then again combined with the rest of the blood and injected directly into the affected area.
- All injections are guided with ultrasound or x-ray to pinpoint exactly where the area of injury is.
Today, PRP treatment near Troy MI is used in mainstream patients for quick preparation and delivery of treatment. Full healing from start to finish takes place in six to eight weeks. However, you should be feeling much better by the second week. Most people just need one treatment but some people, such as those with a severe condition or disease, may require multiple rounds of PRP treatments near Troy MI





Take Advantage of New Advancements in Regenerative Medicine Provided by Board-certified Doctors
Contact Michigan Center for Regenerative Medicine Today and Discover If You are a Candidate. Home Office and Medical Center located at 355 Barclay Cir Suite A Rochester Hills, MI 48307
- PRP Treatment Rochester Hills MI
- PRP Treatment Northville MI
- PRP Treatment Metro Detroit
- PRP Treatment Detroit
- PRP Treatment Novi MI
- PRP Treatment Bloomfield Hills MI
- PRP Treatment Birmingham MI
- PRP Treatment West Bloomfield MI
- PRP Treatment Near You
- PRP Treatment Near Pontiac MI
- PRP Treatment Near Lansing MI
- PRP Treatment Near Grand Rapids MI
- PRP Treatment near Flint MI
- PRP Treatment Near Farmington MI
- PRP Treatment near Downtown Detroit
- PRP Treatment near Milford MI
- PRP Treatment Rochester MI